So as some of you may be aware, I spent the week after my birthday in May stuck in a hospital room because my body decided food was no longer going to go down. My POTS attacks had doubled, I couldn’t stand without nearly collapsing, and at most a piece of toast and a bite of pudding was all I could get down, if it stayed. The nausea and lack of hunger hit a breaking point on Sunday when all I managed was a bite of toast all day. We headed for the hospital Monday mid-morning.
My GI was out of the office for leave for two months and even my Augusta fill in team wanted to throw me on medications and get me in to a hospital for failure to thrive (although apparently that has different meanings across doctors..). Going there didn’t ensure I would get hospitalized and the 3 hours journey was too risky. So we took my cardiologist’s NP’s advice and went to a hospital in their system with the hopes that they would consult my other doctors. Not exactly what happened.
Part 1: getting in
Hospitals are always chaotic but even as a top priority my mom had to hold me upright in my wheelchair for nearly 40 minutes while they found me a room. The fainting wouldn’t stop, the lights were too bright, everything was swimming, and my BP and HR were in chaos. Once we got in the ordered labs but since my port decided not to play nice with blood return, an Iv line was needed in my sideways crooked veins. That shit hurts, even with my amazingly kind nurse. Some labs and urine tests plus 4 more hours later and theres nothing they can detect but they agree to make me an inpatient. I’ve seen the doctor for all of 15 minutes. My nurse decides to log every single medication we pre packed (go mom) into the system before the only person who can leaves. She gets me fluids through my port, more IV zofran than I would like (it rarely works but Iv is the best option when you’ve got benadryl to take in that IV in 20 minutes). Apparently my mom speaking for me since I was so dizzy and weak was noted as “odd” in my hospital notes. It’s not odd. I am in PAIN AND SICK and she’s my advocate whose there to help interpret my gibberish when it starts and prevent a panic. Also that’s a pretty obvious sign of “failure to thrive”.
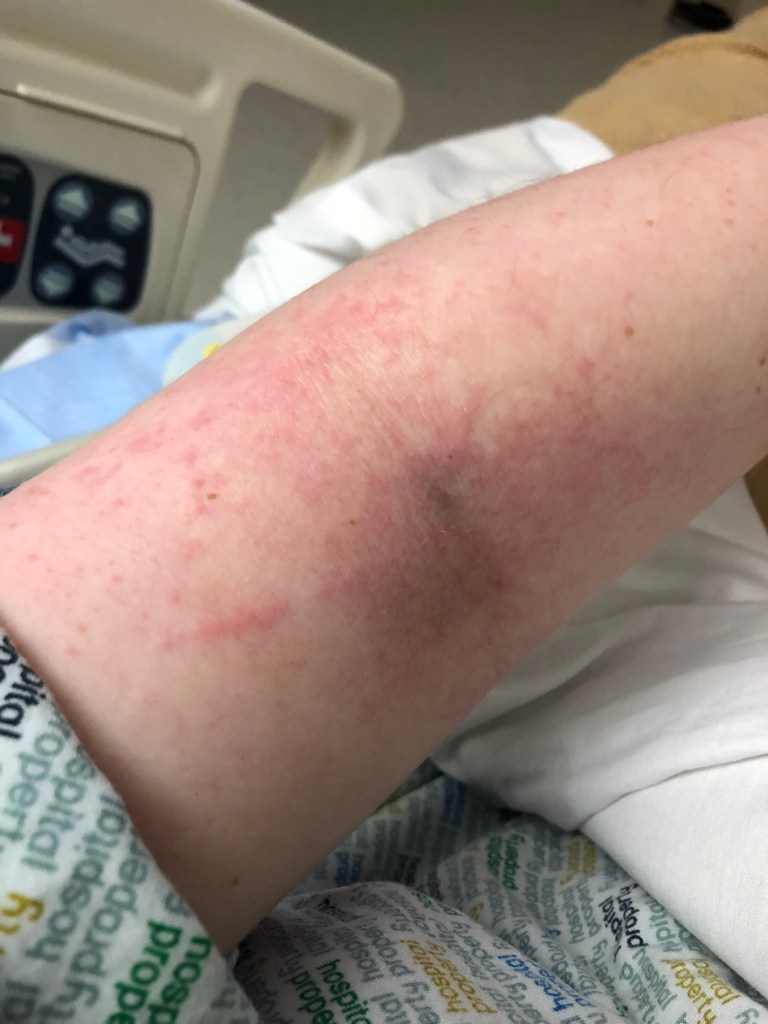
I see another guy for 10 minutes who says they will admit me but want to throw me on reglan. I say not without a GI consult first. As a general note- Reglan is a “standard” for Gastroparesis. It supposed to empty the stomach faster and help with nausea and vomiting. It works in chemo patients but there are SERIOUS black box warnings about this drug. All the other protokinetic drugs like it have been pulled form the market and this one, with my history, means I am high risk for tardive Dyskinesis and NMS (neural malignant syndrome). Add in my general anxiety over new meds in general, and I want to have someone watching me the entire time if I’m taking this. That lovely nurse did get my Iv temp line out and even had pure tegaderm as the dressing but it still left a rash…
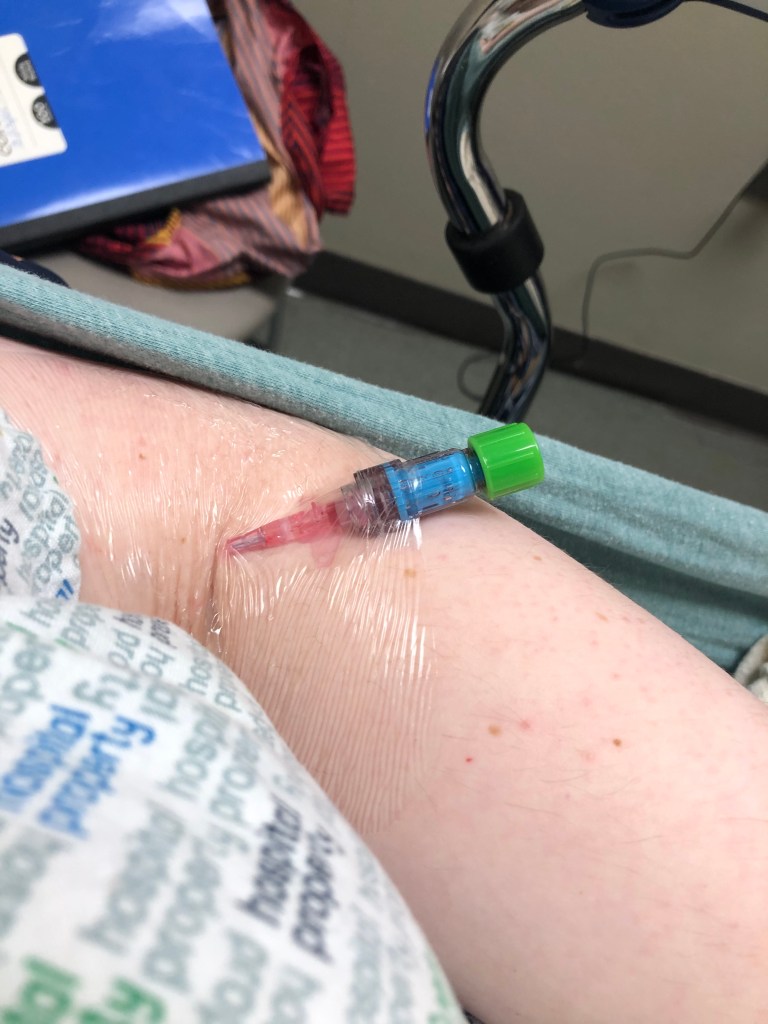
Two X-rays (very efficient techs let em tell you) and one CT without contrast (I know I’m allergic but ya’ll it won’t show much without it…) and we’ve hit the 9 hour mark in the ER. We finally get wheeled up to a room…without a bed.
Part 2- The first night, the medication drama, and a revolving door of nurses in a new wing
They found me a bed. And a broken “recliner” for my mom. Turns out I was placed in a new wing they just opened. Good for my allergies and sensitivities, not so good because we are missing half the important stuff. We have to go through the same song and dance with every single new nurse: “I have a ton of allergies but it will be specific on what’s a topical vs internal problem on my chart you already have. We have all my meds in a box logged and tagged for ya’ll and yes they should stay in here because I have a specific schedule and I don’t know when you’ll get to me (this is a recurring theme FYI). I also can’t walk so what am I going to overdose on or take? Zyrtec? My mom or dad are staying round the clock because you can’t get here fast enough for me to use a bed side commode every time I have to pee and faint. Trust me, I’m a fall risk but we got this worked out to a science. Also I’m a fun disaster”. Every single nurse didn’t want me to not call them to pee but let me tell you, sneezing is a HAZARD with me and I can’t hold it.
They also all eventually conceded and let me do my own benadryl push and take my meds on my schedule after they scanned them since no one has 45 minutes to do a slow IV push of benadryl with me. And I finally got my dextrose Iv bag (complete with reassurances from my ER nurse its corn derived but not chemically related- bless her for taking the time to check)
But 1am hits, my witching hour, and the nausea strikes. The pain is worse and by the time a nurse gets there all they can offer for pain is a giant pill I have to swallow…cut up…while dry heaving…It didn’t stay down and up comes vomit, pill and all with no milk or pudding to help. Cue a hearty Phenergan dose (I hate that on top of my Benadryl) and eventually things calm down.
7Am- rinse and repeat with a new nurse. My meds are late and the lovely ladies of the kitchen have brought me…a fruit platter. Apparently I am listed as diabetic and the giant fruit tray has everything I can’t eat, digest or even be around. Mom practically ran it out of the room so I didn’t see. She had to explain it’s literally plan toast, butter, maybe some chicken soup, or french fries no seasoning. I can’t get anything else down. Fun fact- this song and dance of spectacular meals arriving that I can eat exactly 0 of and more explanations went on the ENTIRE WEEK. The poor kitchen team even knew I couldn’t eat it but doctors kept changing things…without asking.
We finally get my pills down me. I won’t take the new medicine until I see the GI and get a cardiac monitor (As suggested by my amazing psychiatrist who ANSWERED ME ON HER VACATION) and the attending pops in saying she heard I ate a pancake! I didn’t eat a pancake. I took a bite of a single one…Also my meds are listed wrong and we have to get a label reprinted and faxed to the hospital so they will give me the right dose, they don’t have “clearance” to give me my full zyrtec dose, and trying to get my oral suspension valium for my POTS attacks is a hot mess of them trying to find it in their locked fridge (because apparently its a narcotic…).
Dad shows up as we wait on the GI doc who decides to come at 6pm…Mom has not slept in 36 hours by now. We discuss whats going on, review my reglan concerns and agree to a single test dose first to ensure I do okay before we go up to 5mg 3x a day with a swap to oral if I do. The GI is solid, smart, knows of Augusta (he went there for med school) and of my doctors mentor, as well as SIBO. (At the end of all this the dude GAVE me a full round of my antibiotics for the future use because he doesn’t treat it often enough and had samples). I temporarily stop my trulance laxative (BAD CHOICE: by this point i’ve had only one tiny bowel movement in a week and enough zofran and phenergan to stop my gut from moving for a month.
Mom finally goes home for 2 hours of sleep before having to come back. We go in a circle with nurses again until my nurse from the night before shows up and sticks with me.
Part 3: good and not so good nurses
Day 3- its reglan day. I get my cardiac monitor (which they had to wait on because they don’t have enough), we try a single reglan dose amid my shaking pots attack and my dad holding my hand. I don;t remember much of this day or the next but mainly we ran into some issues. Nurses who were sticklers for the clear cut rules, despite us having clearance for everything we had to do and needed. I get to enjoy 4 “it’s all of a reason” and “stay positive” lectures, and my meds schedule is a mess. And my mom keeps being told to go home a rest…but she can’t leave obviously, nor can my dad during the day shift.
This day and part of day 4 involved a bit more frustration. I start my 3 IV doses of reglan. My appetite isn’t back and two bites of potato or soup do not a meal make. The Day 4 adventure was probably the worst. My nurse kept snapping they have a “2 hour window” to admin meds. This meant I got a dose of reglan and then 2 hours later a SECOND dose, hours before I’m supposed to eat. There are air bubbles going into my line. Normal people these aren’t an issue with how small they are. With me? My body will attack them and send me into a flare.
My meds are late again, my POTS attacks are a mess, and I can’t wake up. The reglan sedated me almost completely. My dad and the attending struggled to wake me and the attending took FIVE HOURS to fix a simple medication misprint so I missed out on a dose of meds. My foods been changed AGAIN to fruit platters and the poor food runner is chasing down toast for me…The GI doc decides to lower my reglan dose.
As a general note- nurses are overworked in general. Especially with this new wing and a dozen patients. But beta blockers are a strict schedule you don’t mess with…ever.
But onto the GOOD nurses before I finish day 4’s tale. We had some pretty amazing people care for me. Some who went above and beyond. One was actually there the night I came in and was the charge nurse for my 3rd night. It’s port needle change day for me even though I have a closed circuit with continual fluids, we don’t mess around. She agrees to step up and do the change for me. Somehow she got it perfectly (we brought our supplies) and was amazing. She saw my POTS attack start, complete with a startled tech asking why my blood pressure is so so high after beta blockers. She even called the pharmacist on call to get them to clear me for an extra valium dose to stop the attack.
We had traveling nurses, techs who came to recheck my Bp when I asked, and some really good people who I explained to “I just need someone to look at me while I ave anew medicine or one of these attacks and say ‘medically you are okay, I got you and I am watching over you’.” This was also where I learned the under the tongue valium trick because apparently “like rubbing cocaine into your gums, it absorbs faster!”.
Part 4: The last night, the chaos next door, the really good nurse, and The discharge
Night shift nurse on day 4 was solid but chaos was striking next door. Meds are super late and the nurse is trying to get to me and stay with me while I take my first oral reglan pill. The food order my mom set up earlier has been changed again and I have to have my nurse send in the order to change it…not happening. I’m nauseated and just want the toast but can’t have it because I’ve had none of my Ppi and other meds. Apparently, the ER sent up a critical patient who won;t stop leaving bed next door to me. The charge nurse is trying to wrangle the situation. Alarms are everywhere. She sends a tech to find me actual toast. The lovely kitchen team finds me soup. But the news comes, I go home the next day. My overnight nurse is actually an ICU nurse who is apparently one of the few equipped to handle the hypertensive crisis next door. She’s relieved I am a patient with all my meds laid out and have dad sitting right there to handle anything. However, my cardiac monitor is send off an alarm all night. It isn;t working properly or sticking well or it’s broken despite 4 battery changes. 2Am we get to discover just how stretchy my skin is as they try to pull off monitor tabs. I have red blotches all over and the dang thing is in fact broken…
The next morning, despite all the continued alarms next door (it’s a bed alarm apparently and the guy kept getting out of bed with his BP dangerously high…all day and night) and VERY late meds, I get the best nurse. She’s been trying to get to me and I can just tell this woman had stress radiating off her. I let her vent as we scan my meds. In the span of an hour shes had to chase down two techs, yell at one to stay with Mr. bed alarm, argue with another nurse about medication orders, and chase down a doctor through 3 wings. All while reviewing the note that says “DO NOT LET JESSIE”S MEDS GET MESSED UP”. My dad has to drive a single tagamet over because they don’t stock them and it has to be received by a tech or nurse on my behalf from the front desk. But this woman was fabulous. Curious about my case and I wish I had her every day. Reassuring and calm.
The discharge is started. Cue a mad scramble to get the Reglan oral suspension (which the hospital didn’t have for me to try so now I get to go through the anxiety of trying it at home solo) from any pharmacy, packing up all my crap, and then the POTS ATTACK strikes. They can’t give me any zofran for my car ride home. I never saw the attending who discharged me (although I was charged for more doctors and time then I ever saw them…). At this point I want home. My dad has to come pick us up. My tech helps haul all my crap and load me up.
Part 5: Home
I go home. I have never been so happy to feel car sick and crawl into my bed. That night I have to attempt to choke down the “worlds worst orange juice tang like crap” AKA oral reglan with orange and vanilla flavors…Crying is involved and so is hand holding.
Yet amid all this insanity, people came through. Friends brought my mom coffee every day, the dogs were taken care of one night by one of my best friends, and my dad got to enjoy the hospital food (he claims it was actually good).
Hospitals are my worst fear. If you’ve made it this far then you can tell it was an adventure. It’s a combination of being terrified of being dismissed or labeled wrong, combined with a desperate need for help and a prayer they will do something. My case isn’t clear cut. My Labs drawn daily, by very talented and listening phlebotomists who don’t even question when I point to the exact vein and how to get it, didn’t show much other than my calcium level dropping (pudding and milk based stuff was my main protein source) and my BUN level in the trash. I almost wish something was more clear to help.
I hate the fact that a hospital has the ability for people to communicate between doctors but they don’t (they never called my cardiologist or even my Mast cell specialist) and while they handle crisis or routine, the weird and the wild is uncharted waters. I know I am chaos and not obviously bleeding out, but still… I also hate that nurses are run ragged. Give them two techs and a CNA so they can get stuff done! But most of all, I hate the fact I am already labeled before I walk in the door.
A good friend whose an amazing nurse asked me the other day how to talk to patients with chronic pain as she felt like she didn’t know what was the right thing to say to comfort someone or even say the right thing. Why aren’t there more medical people like her? I offered only the best advice I could, listen. That’s all we want. Nurses are there because they have a care for the human aspect beyond just the medicine. They view a bigger picture yet ca communicate to the medical world in a better way and with more respect given (at least it should be). They are the voices and the comfort we need.
So to end my epic journey on a totally different note: after a few days on reglan we cut it down to 1x a day since it wasn’t helping the nausea or vomiting and I cannot take phenergan with it. Eventually after a really bad day of intense muscle spams and charlie horse level locking, we stopped. The risk was too high and we had gotten me back to some type of eating. Mostly noodle chicken soup and specific cheeses to help me digest food (sorta). But a reset button was hit. Rescue laxatives had to be used multiple times, and my GI finally was back in the office ta few weeks later to review our game plan. Now I get to enjoy a disgusting antibiotic mess (I’ll have to cover that another time because the jury is still out on it).
All in all, I survived a hospital trip. A hugely dreaded adventure and we got some form of reset button hit but long term we still lack a plan.
Stay strong my friends