I actually started this well over a year ago in October of 2023 but stepped away again due to more insanity so….here we go. This is a LONG mashed-up update of sorts. It’s not meant to be negative rather, I’ve begun to untangle the mess that is me in the hopes to slowly accept all the things that have happened over the years. It’s a journey, but part of a journey is learning how to get there.
Has it really been two (3) years since I last wrote something here? Well crap, that’s much longer than a hot minute. I guess there’s a whole lot to cover then right?
Starting out though, two (3) years ago I had to take a step back from writing here, actually writing in general. It was deteriorating my mental health rather than helping me sort through and release some of the emotions surrounding my life. To add to that I was in absolute denial. Denial about just how sick I was. Denial about how badly things were going. Denial about my own mental health. Denial about the realities of the future I was facing. Deny, Deny, Deny.
Mental health has always been a big part of my life. Therapy, among other things, has also been critical, but finding someone, especially during COVID, was impossible. Fortunately I have finally been able to find a therapist who fits right into what I need (SPEAKING OF DENIALS….with absolutely zero help from my insurance who are still kicking and screaming about covering my ABSOLUTELY MEDICALLY NECESSARY THERAPY APPOINTMENTS THANK YOU – just in case someone from UnitedHealthcare happens across this- I fought a year plus battle of unneccesarry appeals and escalations for this…ya’ll owe me) so I can begin the healing process.
Healing maybe isn’t the right word really, recovery? acceptance? adaption? coping? any of those might be a better fit. Really September is just a bad month for me in general and despite my years of denying it, I do have a subconscious fixation on dates when things occurred and it does deeply affect me. But it doesn’t affect me in the ways I thought. One of things I’ve recently learned in therapy is that the subconscious mind does a LOT to protect you. It blocks things out, goes into default mode, deletes, represses, dredges up things, plays tricks on you, the whole enchilada. But it never explains its self to us. So while I might keep saying I’m okay as we approach 6 (yes really six) years since everything imploded, I’m really not. I find myself crying over nothing, not just those cute puppy videos, or sweet family reunion clips. No I’m crying over a hallmark Christmas movie when the tree falls over. I find my heart racing at the notion of needing to make a simple phone call. My thoughts go a million miles a minute and my brain asks me to simultaneously read a book, watch a movie, write, also read this other book, now listen to this news clip, oh and don’t forget about anything critical. Kinda a mess right?
Fortunately, I do know that my body runs in cycles and it will stop, things will calm themselves, and I’ll move on. But the during is the problem. So while I attempt to make a clear update on the past 2 (3) years, i do apologize for the rambling, the wandering, the tangents, and even the strange and dark humor I often find myself surrounded by.
I stepped away from writing in September 2021. I’d been handed Long QT syndrome that summer, GI was absolutely useless at this point, my reactions were flaring all over the place, everything was imploding in a way. I’m having to piece these days together through a few sparse photos of what was going on at the time so hang in there through this adventure. I had a halter monitor test (and reacted for the entire month to those stupid sticky tabs that only told my cardio what he already knew…my hearts fabulous, My POTS is a train wreck, and having to press a button and talk to someone- who then called on call doc- EVERY TIME I FAINTED was…unpleasant for all parties), went in a circle with GI AGAIN, saw my wonderful allergist who gave me IV benadryl and pepcid (honestly its been a life saver and god send over the last few years), managed to get into Vanderbilt Autonomic Clinic for Feb of 2022, and was referred by my allergist to an immunology specializing in Mast Cell (this team is important later so we’ll circle back).
2022 kicked off with a bang. My GI basically gave up and said no to a tube to get me nutrition. My cardio argued my heart developed LongQT from malnutrition but the labs weren’t adding up. Vanderbilt was the most stressful, colossal, expensive waste of time (i could deliver a trilogy on that) but to summarize- I have a mixed type pots (low blood volume, hyper (adrenal dumps) and neuropathic (nervous system signaling sucks). The doc tossed a new med at me (my cardio actually told him about and researched TEN YEARS PRIOR- you’re going to see a pattern here about the team of doctors we’ve been assembling being superior to basically everyone else) and tried to claim half my issues were “functional”. As a general note, that word is thrown in as a way to say “its a mental controllable thing” not what its supposed to mean- we can’t see it yet but the FUNCTIONALITY is impacted in some way NOT controlled by the patient. My allergist and cardio both took offense to the use of that terminology.
Right before we left on the Vanderbilt adventure I did meet my (future) immunologist, hematologist, oncologist who happens to specialize in mast cell issues that go beyond an allergist AND treats with IVIG.
I started my first IVIG treatment the last week of February 2022.
I spent the next 6 months going weekly, then every 2 weeks, every 3, and eventually monthly for infusions as we titrated up. I might tell this tale in more detail in the future but this window of time was absolute hell and a bit foggy for me. As I’ve been told my the nurses who cared for me during infusions and my mother who stayed up all night with me after each infusion in a hotel room screaming, sobbing, and vomiting, it wasn’t a good start. I had rather severe allergic reactions to the IVIG despite steroids repeatedly. Its terrifying. I had aseptic meningitis from the spike in inter-cranial pressure in my cerebrospinal fluid from the proteins in IVIG which left me in so much pain and so sick it was horrifying to witness. I was so weak and unwell I couldn’t hold myself up properly and was fading out mid conversation all the time.
It took months of researching and desperately trying to figure out what could work but eventually (2025 Jessie here- god this was chaos. A lot happened at once) we found a combo of strong steroids, pain medicine, anti-nausea patches (only one doesn’t prolong QT but I’m allergic to the adhesive sooooooo….), and very careful timing of stuff in the right places and I hit the right dose. The goal of IVIG for me is two-fold: Get proteins into the body that can repair the neuropathy damaged nerves basically everywhere and stabilize the POTS/MCAS to some degree since they are feeding each other in an endless loop. It also has the benefit of helping fight illness and infection (guess what? I got to test that theory…a lot…and since I am writing today, it did work).
Amid this chaos my GI situation was crashing even more. I enjoyed being gaslit by yet another doctor (which both of my parents witnessed and were absolutely baffled by. Asking my father for “the facts” over me, the patient? God love him, my fathers a good human but medicine and this type of stuff is wayyyyy out of his comfort zone) and my former GI didn’t believe in J tubes….when your GASTRIC (G) part of the body doesn’t work a G tube is…unhelpful.
ANYWAY, my allergist called a favor in. Pleaded my case with probably the best GI I’ve ever met. He took my case. He was going to retire in a year. I was not likely to be a success. Let me just lay out the facts I later found out. I was crashing fast, nutrition was in the toilet and it had been, for years. I was puking my guts up all day every day. I couldn’t even drink water. I was dizzy and collapsing more and didn’t realize why. (fun fact, anemia makes its debut amid this and has yet to leave) This doctor spoke with me twice and had me scheduled for an NJ tube placement in June the next day.
That tube placement turned into a nightmare. Not because of him, but another doctor decided to be an asshole and give me some glorious MEDICAL TRAUMA AND GASLIGHTING.
Now something contextual you need to understand here is that being someone with a known mental health condition (aka its in my file they get to read), one that frequently get a bad rap and is blamed for nearly everything under the sun, is that taking away my voice, my choice, my right to choose what I want in situations, even the mere suggestion of it, is the single most terrifying thing to me. Present me with the option of standing in front of a tornado or that, and I will choose a tornado any day. Extreme? Absolutely. Probably something I need to discuss with my therapist about? Already on it. But understandable? Maybe not to the average person, but anyone whose been through this knows exactly what I mean. And by taking away I don’t mean necessary intervention for a dangerous or unstable situation, one where you are not capable of going through rational thought. No I mean when you are perfectly capable of making a choice, understanding whats going on, and KNOWINGLY have your voice silenced by someone claiming to know better. Sounds extreme and horrifying right? Yeah. It is.
Back to the hospital stay: Basically the tube feeds triggered allergic reactions to the feeds. Documented, noticeable, seen by multiple nurses and techs and nutritionists who were baffled by them, rashes, hives. Swelling. Itching. Tight throat. Lots of steroids. Took one good pharmacist to go “hey lets keep you on benadryl and pepcid 24/7 until we fix this” to help even a little. But amid that, on a weekend day 3, when I was reacting to yet another feed on no sleep, I had an asshole of a random GI decide that must mean this is now a psych case. This is a whole other story for another time but it was bad enough I am still learning to cope. My new Immunologists office was furious, knowing MCAS and all its complications, and the weekend doctor started calling my hospital at ONE AM demanding to talk to one of the doctors to properly understand what to do. He was ignored. I left the hospital the next day.
My wonderful new GI was pissed. All my doctors were upset. But, at the end of the day, I got my NJ for seven weeks (and only one ER clogged tube adventure on the 4th of July) and eventually found a feed I could have.
August: I was having GJ tube placement surgery to allow feeds and draining of my stomach. That is the important part. Draining has allowed me TO DRINK FLUID AGAIN. AND TRY EATING. AND NOT VOMIT. Holy hell, I woke up and could move but for the first time in YEARS I didn’t throw up. I made it a full 24 hours not puking and sobbed (rather pathetically because my abdomen hurt and the stupid T-tacs that held the tube in place were sewn too tightly. I had to come back a few days later and have a surgeon remove them so i could breath…).
We, as a family, also got to experience terrible home health aids, incredible home health nurses (my nurse joined the team that Summer and has stuck with me since!), and some of the scariest weeks of my life.
The end of September hit and I suddenly got sick. As in, one day sitting up and suddenly I’m shaking, shivering, in pain, my muscles are ripping themselves apart and I cannot breath. A 911 call, confused and concerned EMTs, and a trip to the ER later with blood pressure sky high, heart rate through the roof and no answers….I was told it must be a panic attack….and sent home.
I spent the next 5 days spiking 103-105 fevers daily, my body twisting and shaking while i screamed and either sweat or shook from the cold, and absolutely no help. My GI finally got the message from us and sent me to the ER Friday.
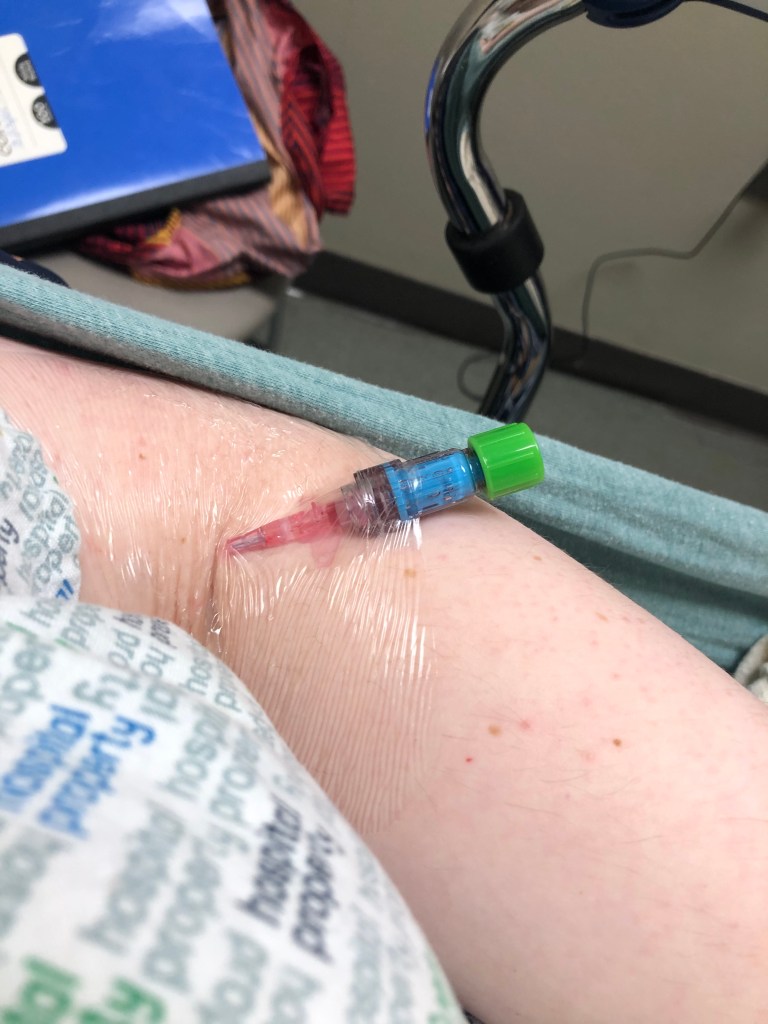
Little side note here: In case you didn’t know, I have a port for all my daily IV fluids and meds. I have had one since 2019. THIS NEXT PART IS IMPORTANT. Fun fact. ANY central line carries a risk of infection. It’s important to monitor the site for that. However, while they may not be the source of an infection, active infections in the body can colonize on your equipment and be essentially impossible to eliminate and thus, you loose the line. ANYONE who has a central line should get to a hospital for testing if a fever above 100.1 appears and its not caused by something like the flu or covid or what not (aka another known fever causing source). Get those cultures ASAP even if it’s a false alarm. Also, somehow, I went to meet and see if a new primary doc would be a good addition to the team…she managed to miss ME BEING ACTIVELY SEPTIC AND FEVERISH BECAUSE SHE WAS MORE INTERESTED IN MY MANY YEARS PRIOR MAN O WAR STING….Rant done.
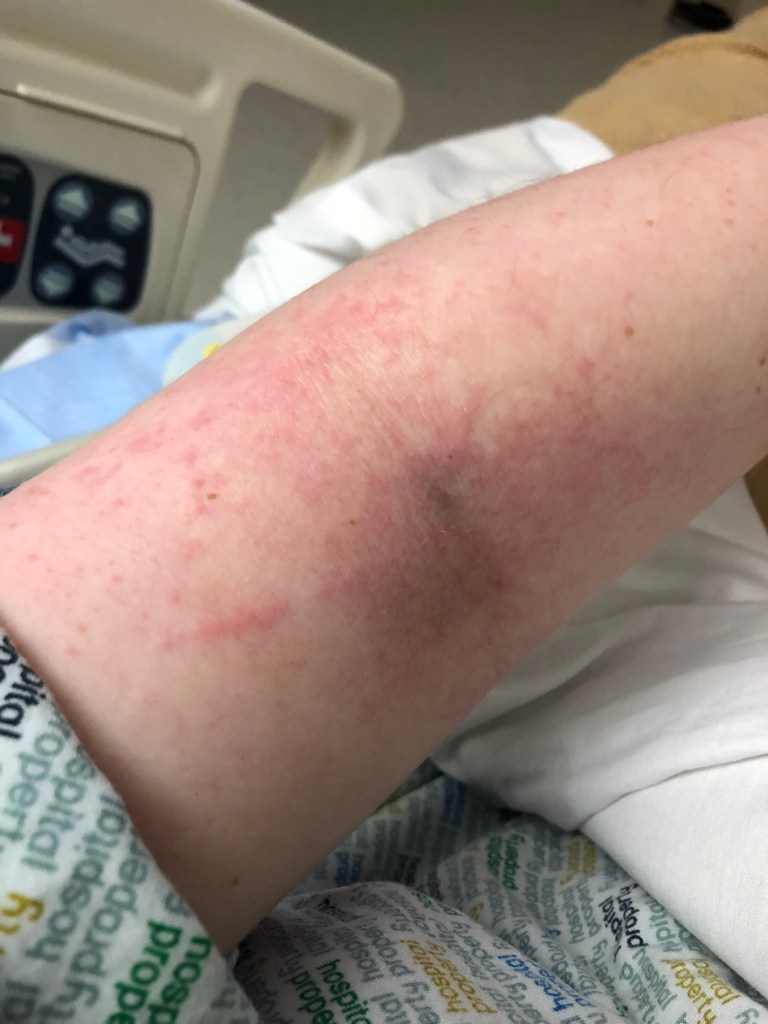
OKAY, back to the adventure. Cue an overflowing ER/hospital (due to county hospitals shutting down) and a 13 hours waiting of me getting progressively worse. I needed a CT scan but due to my contrast allergy from MCAS I couldn’t go without pre-meds. The CT tech wouldn’t do the scan unless I had post scan monitoring in case I had a delayed allergic reaction. There were no rooms for that. I had more blood taken out of me than I can remember (although my destroyed veins and the photos of bruises are enough of a jarring shock to remind me it did in fact happen over and over for the next week). It took the perseverance of my mother chasing down a tech and begging them to prioritize me and check results to get me back into a room.
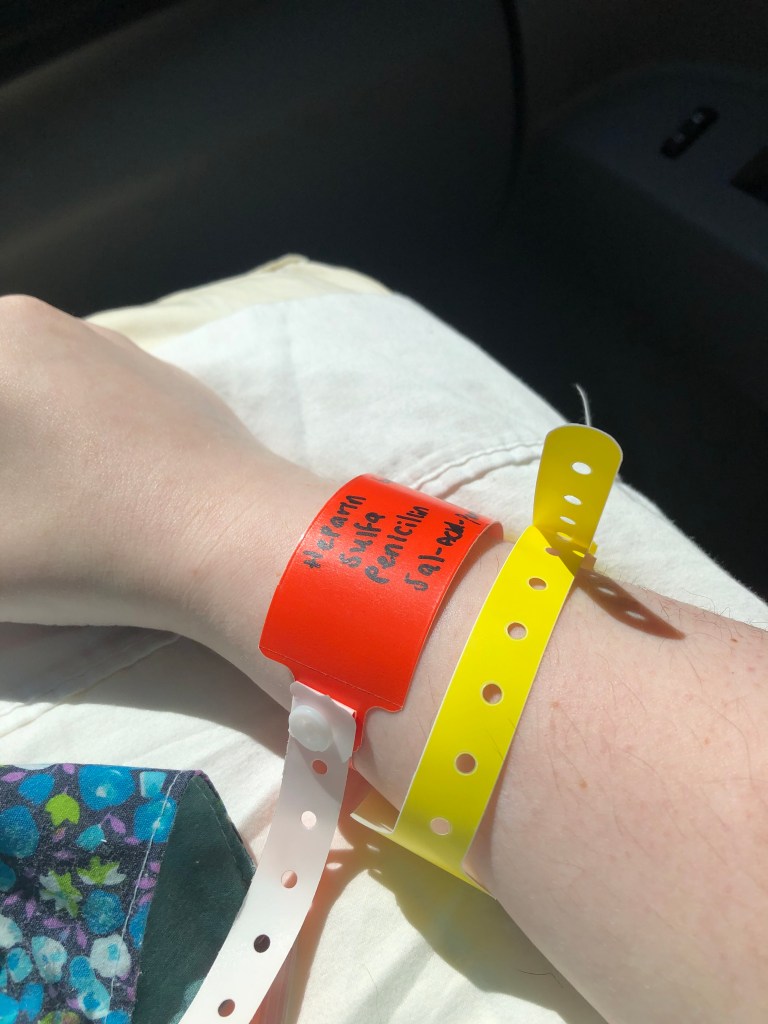
A lot happened fast after that. I was suddenly being given round 2 of pre-meds (since round 1 was hours and hours prior) and hauled off to the scan by that very protective CT tech whose concern about me reacting and demands for me to have a recovery room helped push me into one of the few remaining rooms. During this bleary eyed 3am whirlwind (if you’ve ever been slammed with meds then you know what I mean) I was slammed with undiluted pepcid, benadryl, solumedrol, valium, and god knows what else. They started to try and give me Epi and 2 antibiotics I am allergic to (mom stopped that one by asking what in the ever loving fuck were they about to slam into me without telling me). By the time I got back from the scan the doctor had finally told my parents I was septic with bacteremia and experiencing rigors.
Sepsis is no joke. It’s…terrifying in a lot of ways. I think about it differently because (no surprise here) I’ve been through it twice now, but it’s serious. Turns out that first ER visit they didn’t bother to run cultures, a STANDARD for people with ports and fevers. My labs were terrible. I was anemic to a dangerous level, my red blood cell count was in the trash can, I had insanely low platelets (I learned what LOWLOW meant on a lab report), and the IVIG was the only thing fighting for me. I got thrown on an antibiotic immediately only to learn I was allergic to it the minute my IV benadryl/pepcid bag ran out.
The pharmacist from the disastrous hospital stay just a few months prior made his appearance here and saved they day by putting me on high dose round the clock fluids with lots of benadryl/pepcid. Cue another antibiotic I appeared to tolerate (no surprise here, I did not tolerate it, but I found that out a week later at home), argued with a brilliant but not very “peoply” infectious disease doctor who couldn’t understand why someone with a non-functioning gastrointestinal system plus collapsing veins might need a central line, and got to experience the joy of being WIDE FUCKING AWAKE WHILE MY PORT WAS RIPPED OUT. They don’t sedate you for that no matter how many times you ask nor did they seem to grabs the concept injected lidocaine realllllly doesn’t do much for pain when the surgeon is having to deform and bend the port to rip it out…..I also enjoyed those “surgical meds” slamming me at the same time as my other meds which lead to needing stat team to show up and put me on telemetry because all lovely LongQT was acting up. And my ears got yellowy…I still don’t know why but I’m filing it under “weird shit my body does”.
I had a PICC line shoved in, blew 6 or 7 IV lines, had a staph infection scare, argued about why I shouldn’t be given an iron infusion while on antibiotics, found out my bacteria cultures showed 3 fun gram negative bacteria in my blood, including one from contaminated baby formula…(2 guesses where I might have gotten that from), and enjoyed developing “the most unusual slow-onset allergic reaction I’ve ever heard of” to a whole ass class of antibiotics (this resulted in a Friday afternoon sprint back to the hospital to be monitored while we tried another antibiotic…the one they should have started with…the one WE KNOW IS SAFE FOR ME DAMMIT) and my nurse joined the party again for PICC line care!
As awful as that was, mostly for my family, I was delirious with fever, one good thing came out of it. A surgeon and his team entered my life on the recommendation of the MCAS immunologist. This surgeon and his team have stuck with me since then. They actually listen. And helped get everything sorted to pull out that awful PICC while i was still sedated.
I had a new port placed in November along with iron infusions (needed pre meds for those which is a-typical but hey, no allergic reaction), more IVIG with pre-meds, and on things went. I discovered my hypermobile EDS affects my fibular head in the left knee, aka I subluxed my knee multiple times, got another numb patch. Had scans and testing, only for the orthopedic knee specialist to declare he’d never seen anything that loose, no specialist was suited given my medical BS (genetic factors etc) and offer a useless brace…woo….
Until January. Specifically a holiday weekend my GJ tube, now nearly 6 months old, popped a hole. I needed it to be changed out as it was unusable. Fun fact about tube swaps (because I have had a fuck ton as of writing this), there is a standard procedure they like to use that is…well I’ve found it to be more problematic than helpful. I took my pre-meds, they ran late so my meds were wearing off (this is also where I learned oral Medrol does NOT work to block contrast reactions, IV solu-medrol only works. Medrol just give me anxiety and a heart rate near 200). I informed them about my contrast allergy, they ignored it and said it wasn’t that much I’d be fine. I explained my pain condition and lidocaine not helping and why was it being used in this procedure? They stabbed me with about 20 shots of lidocaine (which backfired because the shots alone trigger my CRPS to flare), then informed me it was to numb the tube site…..
If you read that in order you’ll notice how everything that came out of my mouth was ignored. You’ll see they acted without ever asking or speaking with me. And if you happen to remember just above me mentioning how lidocaine doesn’t work? (My dentist actually figured that out and between him and my podiatrist (who amid all these many months joined the team to help with even more new problems I developed), they came up with a few combos of very long acting meds that work for almost 2 hours on me after giving it 15 minutes to start working and promptly moving through a procedure- they should last 12-24 for normal people…) So you might see a bit of an issue here.
A few more bits about tube swaps, if you don’t like surgical stuff? Skip this. My tube is a dangler so I have a tube hanging out with 3 little tubes with openings at the end all wrapped into 1 larger tube. Larger tube runs into my stomach and uses a balloon ring that sits up against my stomach under the skin holding it in place so my tube doesn’t fall out or flop around. This thing can get stuck if your body tries to eat it and buried bumper syndrome can also occur, aka zero fun and painful. 1 little tube fills that balloon. With contrast water….which, remember, I AM ALLERGIC TO CONTRAST. The 2nd tube stops in my stomach and the 3rd winds down into my intestines. When you swap a tube out you use X-rays to see where it is, insert a guide wire to hold your place, deflate a balloon, yank it out of the bodies small hole (compared to the deflated balloon its…small) and thread a new one in. Inflate, flush contrast, the end.
If you skipped the last paragraph the only important part: There’s a balloon inside me holding the tube, it has contrast water and the balloon can get stuck to the stomach lining. So they start up this whole procedure without listening, deflated the balloon, and yanked. Nothing. Yank. Nothing. Cue aggressive pulling so hard I start screaming and crying. In a NORMAL situation, a surgeon might want to pause and inform the patient whats going on. Adjust the angle. Consider what the problem might be. NOPE. They shove a needle into my tract (the actual hole in me not the tube, down along side it) and pop the damn balloon… More pulling, more yanking, more shoving, contrast. and then they are trying to shove me out a door and I don’t feel right. Allergic reaction starts hitting. I make the nurse turn around and go get someone to give me the damn solu-medrol I informed them about in the first place.
It was a nightmare. I couldn’t sit up or down for a week. I was violently sick from the contrast in me GI system for a full 24 hours. I was terrified now about this whole tube situation. My GI wasn’t pleased but since he isn’t an IR surgeon, he couldn’t do the procedure himself. My infectious disease doc whose been with me through most of this journey sent me a therapist referral immediately when I asked. And insisted I go. Which was probably the best possible move. I developed PTSD from the experience just like my experience in that first hospital stay and had no idea just what that would mean going forward as tube swaps and medical junk was going to always be a part of my life.
I’ll take some time another day to go through just how valuable therapy is for chronic patients of any kind. It can be hard to find the right therapist though. I managed to luck out with someone whose own life experiences happened to make them not only suited for someone like me, but they’re someone who will fight for their patients against anyone and anything.
Fast forward to April 29th and I return from IVIG feeling weird. At least it’s not the tube. A fever appears. It’s an ER visit the following day. We don’t wait. It’s only a few hours to be seen. It’s sepsis. BUT THIS TIME the ER doc actually called my specialist for insight. Didn’t stop me developing Red man syndrome from Vancomycin and add that to the list of allergies but I did only scream and cry for a few hours and had only three episodes of rigors. We also were stuck in the ER all night with no room or meds…the meds I take every day to keep my heart rate and blood pressure stable, and a dozen other things. No one slept.
I turned 28 in a hospital room on antibiotics for one of the same damn gram negatives and a fun little surprise one that had something to do with pink slime mold. I had an even more traumatic port removal, as it took my nurse, on a Thursday afternoon, RUNNING to force them to schedule me after they decided because I asked about a PICC placement to keep IV access to me, this clearly meant I was refusing. So…no scheduling. Again, logic is pretty baffling on this one. I get shoved down there and patronized by some idiotic anesthesia person who asked if i took “my valium today”. I take a very low dose of valium that only helps by taking my Gastroparesis pain/nausea from a 9 to an 8.5…NO THE VALIUM WILL NOT HELP SURGERY STUFF. That idiot and the entire group of morons in the surgical suite decided INSTEAD OF SPEAKING WITH THE PATIENT, to throw a fucking sheet over my head (i shit you not, it happened…i am also very claustrophobic) and use more belts so I “don’t fall off the narrow table”. I would like to point out at this point I had dropped a lot of weight. I hadn’t been able to eat or drink in days, so that was bullshit. I later discovered this procedure was the final straw that made me loose all trust and faith in an medical facility, especially that one.
They did a shit job ripping out that port. I have a huge keloid scar that is migrating and now putting my 3rd port at risk. They gave me random half assed pain meds and LEFT ME POST SURGERY IN A HALLWAY WITH NO SUPERVISION…because the only person on site was a nurse escorting her intubated ICU patient (and her response to being asked to watch the other intubated ICU patient in said hallway she wasn’t responsible for? because the department didn’t bother to call someone to stay with the patient so they decided she should? brilliant. She offered to call the charge nurse to inform them safety policies being violated. No one bothered her again.)
Regardless, it was terrifying to suddenly have meds that are delayed onset hit me, pain strike, and be alone. Bless the transport porter team for being decent and kind people who rushed to come back and get me despite me not being considered a priority. That man stayed with me until my nurse was walking down the hallway towards my room after hauling me back up to my isolation room.
Following that ordeal just a few minutes later, I then got to experience the JOY of a second PICC line placement in the same spot as the first (because why would anyone listen to a patient mentioning their extensive scar tissue….) and spent TWO FULL HOURS having them jam 2 lines in and out of my arm’s blood vessel, while bleeding and crying, and into my heart because one wouldn’t go in properly. My nurse rolled in and poured pain meds into my throat and ignored the failing PICC placement teams protesting, reminding them they were actually late, taking forever, and clearly I was in pain. The portion of the line hanging out of me ended up being so short my PICC stopped working properly after 2 weeks and my immunologist had to scramble to get rush port orders in.
Actually that whole week was a hazy collection of pain from what i do remember. They debated the ICU the first 3 days, I couldn’t tell you why or what was different. My period showed up amid all this, strange GI issues too, on top of my blood sugar going haywire through the roof with no explanation (starvation mode…and steroids…how did no one put that together? especially considering my fingers were BLUE from the number of sticks they performed when i had a perfectly good blood returning line they could have used…).
Basically it was another shit show. And while we are only to May of 2023 with a LOT more to come, I feel I should stop here. This was an important point in my journey, a lost of realizations and hard truths sort of slammed at once.
My GI left medicine at the end of the month. He visited me twice in hospital that week despite having no patients to see or responsibilities there. Our final call I was home recovering and slowly bouncing back. He told me he honestly had his doubts when he met me a year ago that I’d have any type of turn around or success. That there were a lot of odds stacked against my case and even strong patients don’t always make progress.
Somehow I did progress. Somehow I was sitting on the other side of that screen talking to him and discussing a singular improvement in one lab reading. There’s not a cure, there’s not even really a treatment, it’s just management. But he gave me a chance. He gave me a shot when no one else would. So I’m still here.
I’ve been handed off to a good doctor who doesn’t specialize in this. He respected my former doctor and was willing to take my case and help me manage getting feeds and the pump and all my other stuff, but, in his words, “I’m a plumbing guy. I do the manual stuff and leave the brilliance to the smarter doctors on your team. But i can go bang elbows in a pinch!” I don’t think I’ve ever met someone so blunt and honest. It was a little refreshing to not have someone trying to shove their opinion down my throat immediately. (except for Reglan…he hates the medicine with the same burning passion I do except he has a glorious rant) And it made me think about all my experiences in my journey through living in fire.
I wrote this piece below in my journal after my first sepsis round and found it again after coming home from round 2 and added some bits. It felt like I could finally understand what I meant now having gone through everything all over again but with a therapist at least on my team. Today I can look back on it and start to find some bits and pieces that still affect me so much more strongly than I would ever want to admit.
“I don’t think I can really explain the level of guilt and indignity that being this sick, chronically, brings. The discouraging feeling of having yet another specialist insist it’s my own fault for not trying harder or shoving a magic overpriced cure at me. Being asked why am I just not in a hospital with so many problems. These last years I’ve spent more time in hospitals than I would have liked. I don’t think I can explain the feeling of shame from having to ask my father to help me to the bathroom yet again and make sure I don’t fall over along the way. Or asking my parents to come sit with me because I’m anxious over symptoms and then having to ask them to clean up a bucket of vomit 4 or 5 times every day. Waking someone up at 3 am all the time because I’ve gotten sick again. Watching the line of worry turn into lines of exhaustion across my mothers face after 48 hours of no sleep in a hospital together, waiting for someone to do something. Spending the third night with no sleep sobbing from pain, screaming because I have to use a bed pan yet again in hospital and I can’t move properly. Trying not to show just how bad you feel to people who won’t get it by throwing on a fake positive attitude to appease their needs.
Yet I can’t seem to do that facade for my parents. Maybe it’s because they are in the trenches with me. Maybe its because I trust them in all this. Maybe it’s just some subconscious problem and I don’t know it. I don’t want any of it. I can’t fathom being the parent here. I can’t fathom roles reversing. How do I become that strong? I feel like I’m just breaking the most valuable people fighting this fight with me.
But, I have learned one thing through all these years. No one prepares you for this. Nothing can. I don’t think even preparing to become a parent braces you to have to do this for your adult daughter. No training manual or life experience could possibly come close to preparing anyone for this. But, trying to be strong, trying to push through, trying to overcome all those feelings of shame from just living and being forced to ask for help? That is what I can do. I can’t change things, I cannot fix them, but I can try and come to terms with them.”
As I think back on where my mental state must have been, it was rather dim. This was spiral thinking filled with regrets but also a lot of projecting my own issues onto my family. My additions and edits came from a place of starting to recognize where my thinking wasn’t going in a good direction. Loosing trust and faith in medicine, both alternative and standard, hasn’t helped, especially the trust part. It makes it hard to trust in general now. Add in I struggle with acceptance. I was a planner. You think you’re prepared for anything and everything. And along comes the one thing you didn’t plan for, physical limitations your body tosses you. Problems so out of your control you cannot prevent, fix or even really get through it without help. That scares me. The sheer volume (as you’ll see in part 2 of this…) of things every day is overwhelming for THREE people managing it. I look around and realize there isn’t extra help coming. No magical manager of all things is going to swoop into my life and out of sheer kindness step into a support role. No POOF cure is going to fall on me. But, as I am slowly learning, coming to terms with, and accepting the changes I cannot control. It sucks but I think as even more time goes on, I’ll maybe get there.
Stay strong my friends.